Hospital at Home in Germany: opportunities, challenges & prospects
Hospital at Home in Germany: opportunities, challenges & prospects
In Germany, discharge from hospital often marks the end of care. The patient is discharged into a vacuum characterized by unclear responsibilities, a lack of control and high relapse rates. For hospitals, this means unnecessary readmissions, rising costs and dissatisfied patients.
Yet there has long been a better solution - both medically and economically:
Telemedicine technologies and hospital-at-home programs fill the vacuum between inpatient and outpatient care.

Hospital-at-Home: Clinical control without a hospital bed
The challenges in everyday hospital life are well known: rising patient numbers, a shortage of specialists, limited bed capacity. At the same time, hospitals need to ensure a high quality of care - not only during the inpatient stay, but also afterwards.
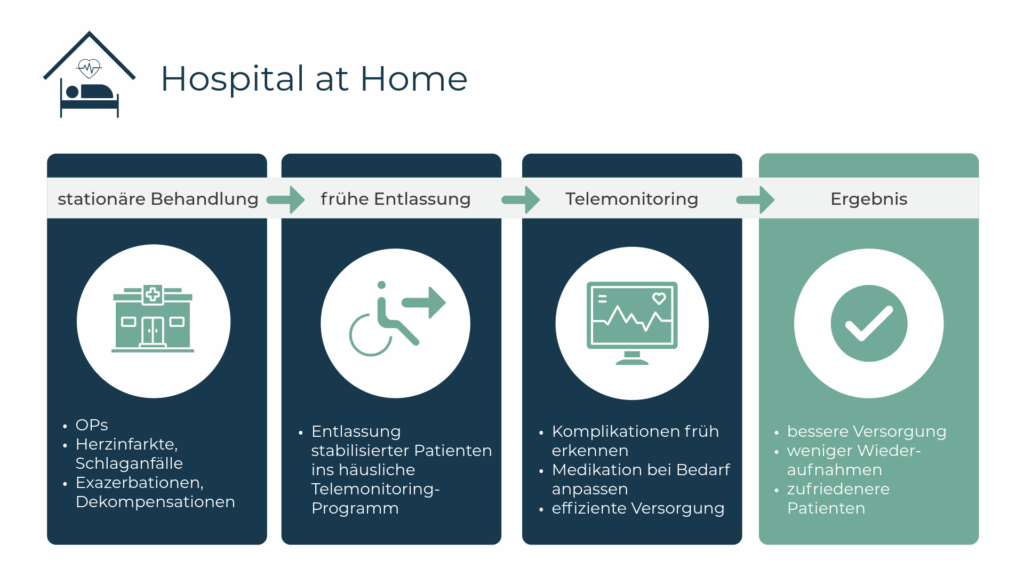
This is precisely where the hospital-at-home concept comes in. It combines three pillars into one equivalent care model in the home:
1. telemonitoring
2. televisits
3. outpatient care
- Digital surveillance (Telemonitoring): Depending on the illness, vital parameters such as blood pressure, pulse or lung function are continuously recorded by the patient and transmitted to the clinic. Automatic alarms are triggered immediately if values become critical.
- Televisits: Regular televisits enable a direct exchange between medical staff and patients - without traveling, but with clinical care.
- Outpatient support on site: If required, mobile care services can make home visits, administer medication or provide nursing care.
The result: Hospital-at-Home enables close-knit, intersectoral and efficient digital aftercare - without a hospital bed, but with clinical standards.
3 reasons why clinics should focus on digital care models now
- The future of patient care is hybrid
Telemedicine hospital-at-home programs enable modern, patient-centric care that brings hospital standards into the living room. Those who invest today are positioning themselves as pioneers in a healthcare system that is increasingly relying on outpatient, digital and flexible care models.
- Resource bottlenecks in clinics require new care pathways
In the face of cost pressure, a shortage of specialists and overcrowded hospitals, telemonitoring programs offer an effective way of conserving inpatient capacity without compromising on quality. Telemonitoring ensures safety and control - even outside the hospital walls.
- Sector boundaries can be overcome digitally
Digital care models such as hospital-at-home promote close collaboration between hospitals, GP practices and outpatient services. Structured task planning and the digital exchange of relevant health data create a seamless flow of information - for more efficient care without frictional losses at the interfaces.
Telemedicine in hospitals: 2 examples from Germany
Example 1:
The Telemedicine Center of the Robert Bosch Hospital cares for patients with chronic heart failure and COPD. The combination of vital data monitoring and personal telephone support enables close follow-up care - with positive effects on quality of life and security of care.
Example 2:
The Institute for Applied Telemedicine (IFAT) of the Heart and Diabetes Center NRW (University Hospital of the Ruhr University Bochum) cares for around 11,000 patients with telemedical services.
With a newly installed telemedical program for the care of heart patients the Institute is setting new standards in telemonitoring for heart failure.
3 ways to finance hospital-at-home in Germany
The implementation of telemedical hospital-at-home programs in Germany can be realized via various financing channels - depending on the strategic orientation and care context:
Regular outpatient HI care via an MVZ
In Germany, telemedical care has so far become part of standard outpatient care for one patient group: the Telemonitoring for chronic heart failure. This approach is ideal for clinics that work closely with an MVZ and wish to transfer inpatients to long-term outpatient care via telemonitoring after discharge.
Selective contracts with health insurance companies
Hospitals and health insurance companies can agree customized care models via individual selective contracts. These contracts offer flexibility in the design of services, remuneration and quality criteria - ideal for innovative hospital-at-home programs that go beyond standard care. They also enable close cooperation between service providers and payers.
Funding via the KHTF (cross-indication)
The Hospital Transformation Fund (KHTF) offers a strategically particularly relevant funding opportunity for the structured establishment of telemedical networks. The central element here is the funding element in accordance with Section 3 (3) KHTFV for the establishment of telemedical network structures.
This subsidy provides targeted support:
- Die Schaffung sektorenübergreifender telemedizinischer Infrastrukturen
- Die Etablierung digitaler Versorgungsketten zwischen Klinik, niedergelassenen Ärzten und ambulanten Diensten
- Investitionen in interoperable Telemonitoring-Systeme und digitale Kommunikationsplattformen
Der entscheidende Vorteil: Die Förderung ist indikationsübergreifend ausgelegt – Hospital-at-Home-Strukturen können somit in verschiedenen Fachbereichen der klinischen Nachsorge geschaffen werden. Das schafft nachhaltige, zukunftsfähige Versorgungsstrukturen, die über einzelne Krankheitsbilder hinausgehen.
Krankenhäuser, die jetzt den Aufbau telemedizinischer Netzwerke strategisch angehen, sichern sich nicht nur Fördergelder, sondern positionieren sich als zentrale Akteure in einer vernetzten, digitalen Gesundheitsversorgung.
Quelle:
1 Bundesministerium für Gesundheit: Krankenhausversorgungsverbesserungsgesetz (KHVVG)
In die Zukunft der klinischen Nachsorge
Die Telemedizin-Plattform SaniQ OS ermöglicht Kliniken eine strukturierte, digitale Nachsorge – für frühere Entlassungen, weniger Wiederaufnahmen und zufriedenere Patienten.
These articles might interest you:

Zukunftscheck: Telemonitoring in Deutschland
Telemonitoring ist als digitalmedizinische Schlüsseltechnologie zentral, um drängende Herausforderungen im deutschen Gesundheitssystem zu bewältigen. Wo also steht Deutschland bei der Integration dieser zukunftsweisenden Technologie in die Gesundheitsversorgung?

Wie digitale Medizin die Versorgungslücke bei Seltenen Erkrankungen schließt
Innovative Anwendungen aus der Telemedizin können die Versorgung von Menschen mit Seltenen Erkrankungen entscheidend verbessern. Ein Ärztinnen-Team der Berliner Charité geht neue Wege, um den Betroffenen einer neurologischen Erkrankung die dringend benötigte Unterstützung zu bieten.
